Health policies and data
Paying providers for healthcare
|
Healthcare provider payment systems across OECD countries are undergoing a paradigm shift. Payers for healthcare are moving from having a passive role when reimbursing providers to pursuing a variety of policies as part of broader efforts to improve the quality and efficiency of care. How health providers are paid is one of the key policy levers that countries have to drive health system performance. |
|
KEY PUBLICATIONS
 |
Value-based providers’ payment models: understanding where and under which conditions they work Released August 2022 The report “Value-Based Providers’ Payment Models: Understanding where and under which conditions they work” explores the bundled payment model and offers country case studies examining the application of this model in a real-world context. |
 |
Better Ways to Pay for Health Care Released June 2016 Payers for healthcare are pursuing a variety of policies as part of broader efforts to improve the quality and efficiency of care. Payment reform is but one policy tool to improve health system performance that requires supportive measures in place such as policies with well-developed stakeholder involvement, information on quality, clear criteria for tariff setting, and embedding evaluation as part of the policy process. Countries should not, however, underestimate the significant data challenges when looking at price setting processes. Data access and ways to overcome its fragmentation require well-developed infrastructures. Policy efforts highlight a trend towards aligning payer and provider incentives by using evidence-based clinical guidelines and outcomes to inform price setting. There are signs of increasing policy focus on outcomes to inform price setting. These efforts could bring about system-wide effects of using evidence along with a patient-centred focus to improve healthcare delivery and performance in the long-run. |
OECD PROJECT ON PAYMENT SYSTEMS
There has been increasing experimentation with new ways of paying providers. In primary care, payments have become more blended as countries seek to combine different elements of payments as incentives to meet specific objectives. Countries that have used capitation and budgets have added elements to drive quality or increase productivity. In hospitals, many OECD countries have introduced DRG payments alongside other policies to constrain overall budgets and stimulate competition, with a focus on productive efficiency. Over and above these broad trends, there has been increasing experimentation with new ways of paying providers especially payment systems that span across levels of care. In this context it is worthwhile to take stock of payment systems in the OECD and highlight promising innovations that could help shed light on how governments might pay for health in the coming years.
The OECD project’s objectives are as follows:
- 1. Profile payment methods used in OECD countries and assess their impact on quality and costs;
- 2. Analyse recent innovations in payment systems;
- 3. Analyse challenges in implementation of new payment methods.
The OECD project is supported by a group of experts from participating OECD countries.
CURRENT PROVIDER PAYMENT IN OECD COUNTRIES
|
In many countries payment systems have evolved beyond fee-for-service and budgets. In primary care, additional payments linked to improvement in health outcomes or to encourage gate-keeping or care co-ordination have become increasingly popular. In hospitals, there has been a shift to finance services on the basis of activity using diagnosis-related groups (DRGs). The 2012 Health Systems Characteristics Survey analyses the payment modes currently in use in OECD countries to remunerate primary care, outpatient specialist care and inpatient care, the price regulations for health services and identifies new innovative modes of payments in more detail. |
|
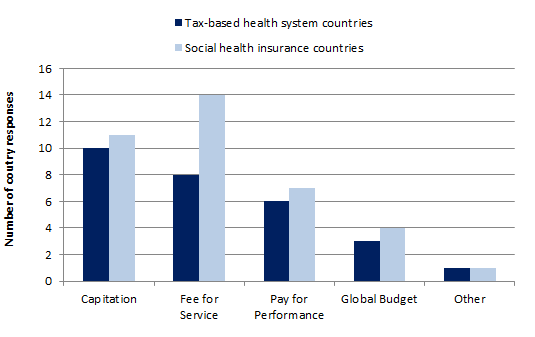
Mode of payment and financing in primary care Source: OECD Health Statistics 2013, Health Systems Characteristics Survey 2012, and Secretariat's estimates. Information as of April 2014. |
PUBLICATIONS
- Purchasing for Quality Chronic Care - Summary Report, WHO-OECD (October 2023)
- Value-based payment models in primary care: An assessment of the Menzis Shared Savings programme in the Netherlands, OECD Health Working Paper No. 157 (June 2023)
- Innovative providers’ payment models for promoting value-based health systems, OECD Health Working Paper No. 154 (April 2023)
- Value-based providers’ payment models: understanding where and under which conditions they work (August 2022)
- Better Ways to Pay for Healthcare (June 2016)
- Health Institutional Characteristics: A Survey of 29 OECD Countries, OECD Health Working Paper No. 50 (April 2010)
 |
Paying for Performance in Healthcare: Implications for Health System Performance and Accountability The detailed analysis of these 10 case studies together with the rest of the analytical text highlight the realities of P4P programs and their potential impact on the performance of health systems in a diversity of settings. This book provides critical insights into the experience to date with P4P and how this tool may be better leveraged to improve health system performance and accountability. Released September 2014 > Subscribers and readers at subscribing institutions can access the online edition via the OECD iLibrary > Click on the cover for a free preview |
ACCESS THE DATA
- Modes of payment in primary care
- Modes of payment for outpatient specialist services
- Modes of payment for inpatient care
CONTACT US
- Mr. Michael Mueller: michael.mueller@oecd.org
- Mr. Luca Lorenzoni: luca.lorenzoni@oecd.org
- Ms. Emily Hewlett: emily.hewlett@oecd.org
- health.contact@oecd.org
 Follow us on Twitter via @OECD_Social
Follow us on Twitter via @OECD_Social
Back to the Health System Characteristics homepage
Related Documents