Health
Health Systems Resilience
|
The COVID-19 pandemic has led to massive societal and economic consequences across OECD countries and beyond, including millions of deaths, reduced life expectancy and long-lasting health impacts. The pandemic has put health systems under extreme stress; they have had to adapt to changing circumstances while continuing to provide high quality healthcare. Ongoing and future challenges, such as antimicrobial resistance and climate change, also require resilient health systems. The OECD is providing policy insights and guidance to improve health system resilience. |
|
READY FOR THE NEXT CRISIS? INVESTING IN HEALTH SYSTEM RESILIENCE
 |
Released 23 February 2023 The COVID-19 pandemic had massive consequences for societies and health systems across the OECD and beyond. Health systems were not resilient enough. Resilient health systems plan and are ready for shocks, such as pandemics, economic crises or the effects of climate change. They are able to minimise the negative consequences of crises, recover as quickly as possible, and adapt to become better performing and more prepared. Smart, targeted investments in health system resilience are needed to improve health and ensure the next shock is less disruptive and costly.
|
WHAT is resilience and why is it important?
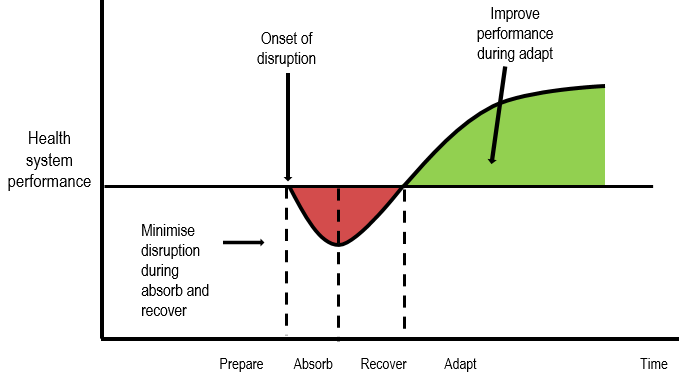
Health system resilience is the ability of health systems not only to prepare for shocks, but also to minimise the negative consequences of such disruptions, recover as quickly as possible, and adapt by learning lessons from the experience to become better performing and more prepared. Resilience calls for a multidisciplinary approach, which the OECD has adopted.
- Find out more about The New Approaches to Economic Challenges (NAEC) initiative
The disruption cycle: the four stages of a response over time
Sources: Adapted from OECD (2019), “Resilience-based Strategies and Policies to Address Systemic Risks”, and National Research Council (2012), Disaster resilience: A national imperative.
Discussions between countries, experts and other stakeholders
|
|
FINANCING RESILIENT HEALTH SYSTEMS: IS THERE A TRADE-OFF BETWEEN EFFICIENCY AND RESILIENCE? Following the COVID-19 pandemic, countries are looking to build more secure and resilient health systems, to be better prepared for future crises, and mitigate future pandemic related economic costs. However making the best investment decisions, and ensuring finance ministries support, at a time of constrained public expenditure will be very challenging. Closer collaboration between Finance and Health Ministries is needed, including the development of multi-year commitments, to enhance both efficiency and resilience while reducing waste in health systems. Smart investments in health resilience can protect economies from destabilising shocks, and protect people from premature death. The challenge, which will be a point of discussion during this year’s OECD Ministerial Council Meeting, is to make these necessary investments whilst maintaining the financial sustainability of health systems. This webinar, supported by the NAEC Initiative, discussed how to incorporate such resilience thinking within a comprehensive strategy for high-performing, sustainable health systems. |
Resilience testing
- The European Commission’s Expert Panel on effective ways of investing in health recommended resilience testing of the health systems of European Union Members. The EU4Health Programme is funding joint work between the OECD and the European Observatory on Health Systems and Policies to test resilience scenarios and produce a handbook.
- Read Strengthening Health Systems: A Practical Handbook for Resilience Testing (March 2024)
Evaluations
As countries seek to learn from the COVID-19 crisis and increase their resilience for the future, evaluations are important tools to understand what worked or not, why and for whom.
- Evaluation of Luxembourg's COVID-19 Response - Learning from the Crisis to Increase Resilience, (November 2022)
KEY DATA
Note: Based on annual reported totals of deaths from all-causes. Age standardised mortality rate uses the 2015 OECD Standard Population.
Information on data for Israel.
FURTHER READING
- Evaluation of Belgium’s COVID-19 Responses - Fostering Trust for a More Resilient Society (December 2023)
- Primary Health Care for Resilient Health Systems in Latin America (December 2022)
- Evaluation of Luxembourg's COVID-19 Response - Learning from the Crisis to Increase Resilience (October 2022)
- The health impact of COVID-19, in Health at a Glance 2021: OECD Indicators (November 2021)
- How resilient have European health systems been to the COVID-19 crisis?, in Health at a Glance: Europe 2020 - State of Health in the EU Cycle (November 2020)
- "Curing vulnerabilities", article by Francesca Colombo, in The Global Governance Project (October 2022)
- "We must invest more in health systems to foster recovery and build resilience to future shocks", article in the Commonwealth Health Report 2022
- Pathway to UHC: Three priorities for stronger, more resilient, more inclusive health systems, World Bank Blogs (December 2021)
- "Enhancing co-operation to create better health policies for safer and healthier lives", article in The European Files, Towards a European Health Union, May-June 2021 issue
- Pandemic Scenarios: Number crunching and communication strategies”, Blog, The OECD Forum Network, Tackling Coronavirus (COVID-19): contributing to a global effort (July 2022)
- Resilience of Health Systems to the COVID-19 Pandemic in Europe: Learning from the first wave, Blog, The OECD Forum Network (November 2020)
- Resilient health systems: What we are learning from the COVID-19 crisis, Blog, The OECD Forum Network (April 2020)
- New Approaches to Economic Challenges (NAEC) work on Resilience
- Visit the OECD hub on Building a resilient recovery
- Read about The impact of COVID-19 on health and health systems
- Health Statistics
- Health Policies
- Health Publications
CONTACT
For more information, please contact health.contact@oecd.org

Follow us on Twitter @OECD_Social
Related Documents